Spine Physiotherapy refers to the rehabilitation of any spine-related injuries. Spinal physiotherapy also deals with the treatment of any pain in the back, neck, or head.


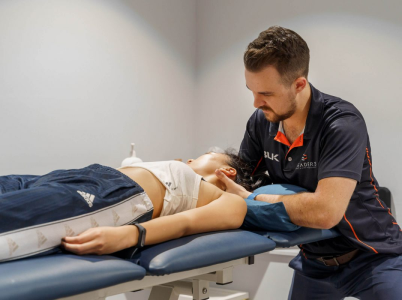
Neck pains are very uncomfortable for anybody. The good news is that because the neck area has a lot of blood vessels, it has a lot of blood flow, thus it heals and recovers relatively quickly. Physiotherapy can help hasten the healing process by determining the cause of the neck pain and treating the area specifically rather than simply using hot or cold treatment. Whether it’s acute or chronic neck pain, physiotherapy can help improve pain-free range of motion and alleviate some painful symptoms and movements.

The thoracic spine is where our ribcage is attached. Joints called the costovertebral joints connect the proximal end of the ribs to its corresponding thoracic vertebrae. Physiotherapy is generally considered the best course of action when you have costovertebral joint sprains and irritations. During your Physiotherapy consultation you will be treated with a variety of modalities that includes manual therapy and soft/deep tissue release. Our team of Physios will also be able to provide you with some advice and education around ways to prevent re-aggravation and re-injury in the future.
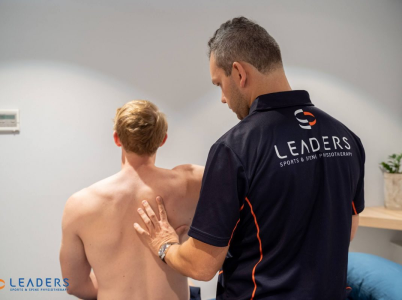
Thoracic Outlet Syndrome (TOS) is a term used to describe three related syndromes involving the compression of nerves, arteries, and veins in the lower neck and upper chest area. These can cause pain through the arm, shoulder, and neck. The diagnosis of TOS can be complicated for all health professionals as there are many conditions that have similar symptoms. We can help you get an accurate diagnosis to be able to treat your condition accordingly. Our state-of-the-art facility is one of the best in Brisbane CBD, so you can rest assured that we got you covered.
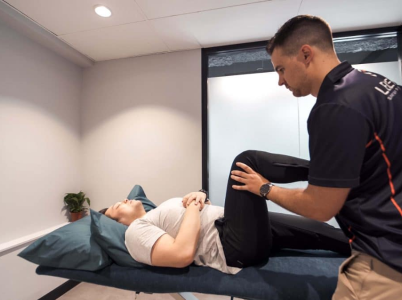
Sciatic pain, or sciatica, is a blanket term used for ongoing leg and potential foot pain, originating from the lower back or glute area. Symptoms may vary from person to person depending on the cause and severity of the condition. At Leaders Sports & Spine Physiotherapy we pride ourselves in preventing people from spending the rest of their lives taking medications. Our team has extensive experience in dealing with sciatic and other spine conditions, and understand where Physiotherapy can help or when surgery is the more appropriate course of action for your condition.

Scoliosis is the lateral (sideways) curvature of the spine, most of which are mild cases with little to no symptoms. The mild cases of scoliosis can be treated by a Physiotherapist. The assessment will involve the checking of the movement and mobility of the spine along with the surrounding musculature and functional abilities. After a thorough assessment, our physios can recommend a program for the treatment and rehabilitation of the spine and its surrounding joints and muscles.